Protesi Fissa
Il manufatto protesico deve essere adeguatamente integrato dal punto di vista biologico rispettando sia i tessuti gengivali che l’organo pulpare durante le fasi di preparazione dentale, presa d’impronta, posizionamento del provvisorio e cementazione dei restauri.
La perdita di elementi dentali o la mancanza di affidabilità degli elementi naturali esistenti porta il clinico ed il paziente a scegliere il più delle volte soluzioni protesiche ancorate ad impianti osteointegrati, che possono efficacemente rimpiazzare gli elementi mancanti.
In qualsiasi riabilitazione protesica, sia limitata a un settore del cavo orale sia che estesa alla bocca intera, risulterà di importanza fondamentale per il mantenimento nel tempo dei restauri realizzati, un periodico e scrupoloso monitoraggio della riabilitazione eseguita, così come un attento e sistematico controllo dell’igiene orale del paziente.
HAI BISOGNO DI MAGGIORI INFORMAZIONI?
PRENOTA
UNA CONSULENZA
Cause della mancanza di un dente:
- L’elemento dentale è stato estratto poiché attaccato pesantemente dalla carie che ha determinato una pulpite non curata per tempo e il paziente ha deciso di sostituirlo con un ponte;
- a causa della frattura traumatica (incidente) non solo della corona ma anche della radice del dente;
- ascesso dentale importante;
- vecchiaia;
- parodontite grave che ha determinato l’instabilità dell’elemento dentale che il dentista ha dovuto provvedere ad estrarre.
Perché sostituire il dente mancante?
- Per ripristinare la corretta masticazione;
- per impedire lo spostamento dei denti adiacenti provocando malocclusioni;
- per ripristinare l’estetica del paziente che si sentirebbe a disagio nelle sue relazioni sociali;
- nel caso dell’impianto dentale, esso contribuisce a ritardare notevolmente la regressione dell’osso.
Corone Dentali
Le corone dentali sono protesi fisse realizzate in vari materiali:
- ceramica (porcellana pura)
- zirconio
- metallo-ceramica (lega-ceramica)
- metallo-resina
- metallo
- resina (di solito sono corone provvisorie)
Quando sono consigliate le corone dentali?
- Quando i denti sono affetti da carie, sono scheggiati o rotti e non possono essere ricostruiti con delle otturazioni;
- quando i denti sono devitalizzati, perché dopo la devitalizzazione diventano deboli e possono rovinarsi;
- quando i denti sono colpiti da malattie che ne stanno distruggendo lo smalto;
- quando dobbiamo ricoprire un impianto.
Le moderne corone sostituiscono le vecchie corone in metallo che hanno come svantaggio più grosso la mancanza di traslucenza a livello gengivale, poiché i raggi della luce incidente, diversamente dal dente naturale, vengono bloccati dalla presenza del metallo sottostante e questo, anche in corone ben eseguite, provoca frequenti inestetismi.
La zona di finitura capsula-dente, inoltre, è costituita da un bordino metallico, spesso rivestito da un materiale opacizzante, che traspare attraverso la gengiva rovinando la naturalezza del sorriso. Questi problemi, associati alle esigenze estetiche sempre crescenti della nostra epoca, hanno portato a produrre corone in ceramica integrale o in zirconio che hanno permesso di ottenere risultati eccellenti proprio perché, prive di anima metallica, riproducono la trasparenza del dente naturale.
Il trattamento
Prima di procedere con l’incapsulamento, il dente viene preparato. La preparazione del dente include le seguenti tappe:
- quando richiesto il dente viene devitalizzato, per evitare sofferenze e dolori;
- successivamente il dente viene levigato, fino ad ottenere lo spessore necessario per l’incapsulamento (ovviamente la parte di dente asportata sarà pari allo spessore della corona da montare);
- si prende l’impronta, si sceglie il colore e si procede con la preparazione della corona artificiale;
- l’ultima tappa sarebbe la cementazione della corona dentaria definitiva (se nel frattempo è stata applicata una corona provvisoria). La corona può essere cementata con uno specifico cemento dentale che funge anche da sigillante per tenere ben salda e ferma la corona.
Il trattamento è indolore. La corona sarà realizzata per essere uguale agli altri denti e la tonalità di colore dei denti vicini sarà utilizzata per fare in modo che la corona si inserisca il più naturalmente possibile tra gli atri denti.
Una corona provvisoria, normalmente realizzata in materiale plastico, sarà montata sul dente preparato in attesa che la corona definitiva sia pronta. Questi provvisori potranno essere meno naturali della corona definitiva e quindi si potranno notare maggiormente ma dobbiamo ricordare che sono realizzati per durare solo poche settimane.
Ponti
Il ponte dentale è una protesi fissa che serve per la sostituzione di uno o più denti che mancano per differenti motivi. Per ripristinare la funzione masticatoria ottimale e l’estetica, l’odontoiatria propone due soluzioni:
- ponte sorretto da denti adiacenti che fanno da pilastri;
- corona su un impianto dentale osteointegrato che funge da radice artificiale su cui assicurare una corona protesica.
Spetta al dentista valutare il caso in esame e descrivere al paziente i vantaggi e gli svantaggi delle due procedure odontoiatriche.
A differenze dell’impianto, che implica l’inserire una vite nell’osso gengivale con sopra un dente artificiale, il ponte è un dente artificiale privo di radice, che viene appoggiato direttamente sulla gengiva dove un tempo era presente il dente naturale. Il dentista lo ancora poi ai denti contigui.
Qual è la procedura per applicare un ponte dentale?
Durante la prima visita, i denti pilastro sono preparati. La preparazione implica un recontouring di questi denti rimuovendo una porzione di smalto per lasciare spazio a una corona sopra di essi. Successivamente, viene prelevata l’impronta dei denti che serve come modello da cui il ponte, elemento intermedio, e le corone saranno creati da un laboratorio dentale.
Viene poi realizzato il provvisorio in grado di donare da subito comfort e protezione dei denti e delle gengive esposte mentre è in corso la preparazione del ponte definitivo.
Il provvisorio, inoltre, permette di modellare e condizionare la forma gengivale e di previsualizzare il risultato finale: il lavoro definitivo è di fatto la copia del provvisorio.
Successivamente, verrà presa un’impronta di precisione che sarà consegnata all’odontotecnico per effettuare tutte le dovute prove estetiche e funzionali. Il ponte potrà quindi essere cementato.
Possono essere effettuate visite multiple per verificare l’adattamento della struttura metallica e soprattutto il morso.
Ricordiamo che i ponti dentali richiedono un’igiene domiciliare scrupolosa. Per evitare malattie paradontali e carie, lo spazzolamento accurato dei bordi gengivali e dello spazio al di sotto del ponte sono indispensabili; inoltre, la zona dove è posizionato il ponte dovrà anche essere pulita attraverso il passaggio di uno specifico filo interdentale – superfluoss – al fine di evitare che residui alimentari possano innescare infezioni, ascessi, infiammazioni o qualsivoglia processo patologico.
Intarsi
Gli intarsi hanno preso il posto delle vecchie amalgame, ovvero delle otturazioni dentali grigie, i cosiddetti piombaggi che oltre ad avere un bruttissimo impatto estetico, contengono il 50% di mercurio, un grammo del quale è sufficiente a contaminare 20.000 kg di alimenti (normativa vigente CEE).
Il pericolo delle vecchie amalgame dentali consiste essenzialmente in un’esposizione cronica a bassi livelli di mercurio che interessa, secondo recenti studi epidemiologici, il cervello, la tiroide, il midollo osseo, i reni, il fegato, il cuore ed altri tessuti.
Gli intarsi sono di fatto delle otturazioni in composito o ceramica, eseguite in laboratorio, che vengono poi cementati nella cavità del dente, precedentemente preparato.
Si utilizzano per i denti posteriori (premolari e molari) dove è più facile che le cavità siano di grosse dimensioni. Il dente viene preparato come per un’otturazione che, invece di essere effettuata dal dentista, viene eseguita dal laboratorio odontotecnico su un’impronta di precisione. L’intarsio viene poi cementato.
Oggi l’utilizzo degli intarsi in composito o ceramica integrale rappresenta l’opportunità di limitare l’invasività delle metodiche restaurative, mantenendo i margini del restauro fuori dal solco gengivale e ripristinando efficacemente le caratteristiche biomeccaniche degli elementi trattati.
Gli intarsi hanno una resa estetica molto elevata, durano nel tempo e il punto di contatto tra intarsio e dente è più preciso rispetto all’otturazione normale.
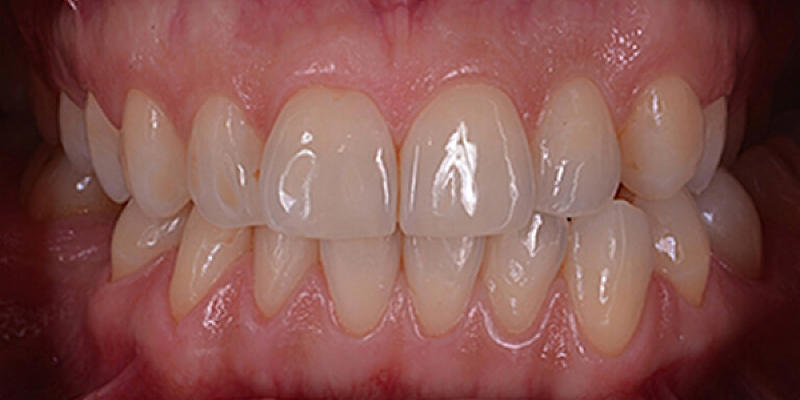
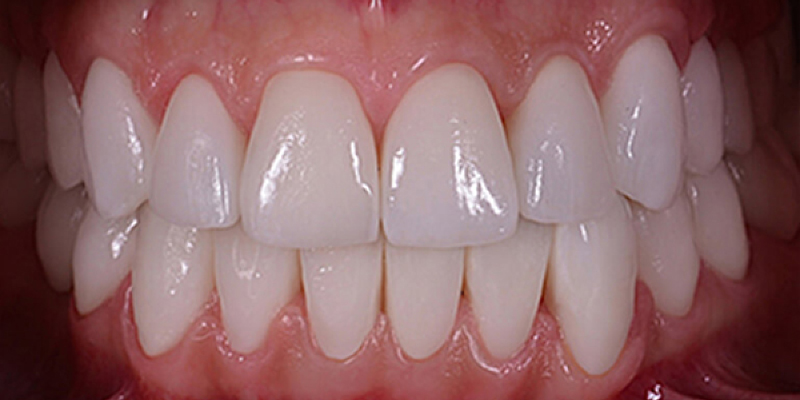
I MIEI
RISULTATI
perfetto, ma so che esiste il
sorriso perfetto per ognuno.
